
Green Sickness: A Historical Look at the 'Disease of Virgins'
Explore the mysterious disease of virgins that shaped medical control over young women from the 1550s to 1920s through marriage and motherhood.

The Medicine behind food – from starters to desserts
Discover why we eat soup first and cheese last—the humoral theory and Renaissance medicine shaped our modern meal structure.

Why Do We Picture Witches as Old Women?
Why are witches always old women? Explore how menopause, humoral theory, and misogyny shaped the witch stereotype from medieval times to today.

Green Sickness and Virginity
Discover green sickness, the mysterious ailment that affected young women from the 1550s to 1920s—diagnosed by paleness, fainting, and virginity.
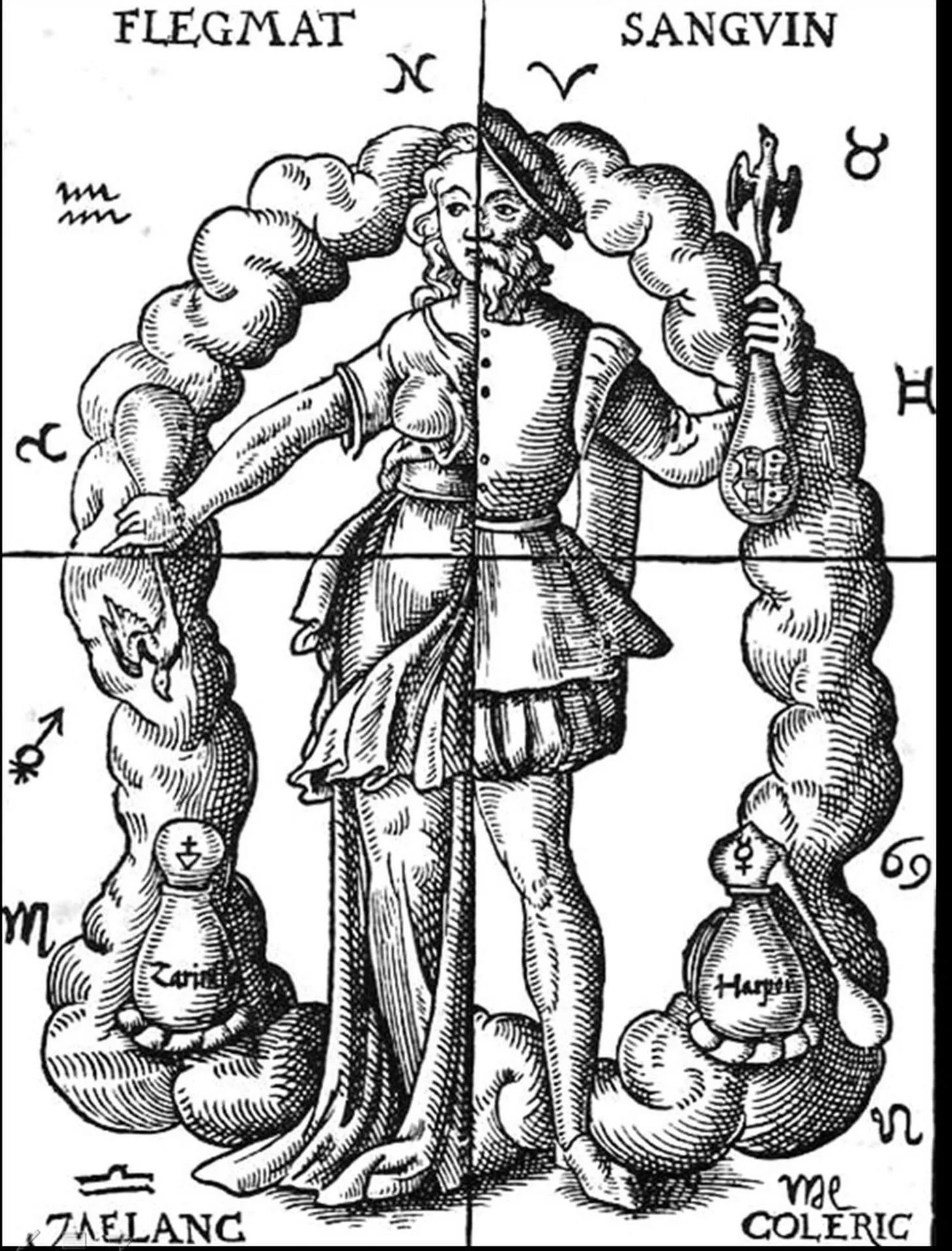
Humoral Theory: How the Four Humours Shaped Medicine for 2,000 Years
Blood, phlegm, yellow bile, and black bile — the four humours formed the foundation of Western medicine from ancient Greece to the 18th century.

Green Sickness: A Historical Look at the 'Disease of Virgins'
Explore the mysterious disease of virgins that shaped medical control over young women from the 1550s to 1920s through marriage and motherhood.

The Medicine behind food – from starters to desserts
Discover why we eat soup first and cheese last—the humoral theory and Renaissance medicine shaped our modern meal structure.

Why Do We Picture Witches as Old Women?
Why are witches always old women? Explore how menopause, humoral theory, and misogyny shaped the witch stereotype from medieval times to today.

Green Sickness and Virginity
Discover green sickness, the mysterious ailment that affected young women from the 1550s to 1920s—diagnosed by paleness, fainting, and virginity.

Humoral Theory: How the Four Humours Shaped Medicine for 2,000 Years
Blood, phlegm, yellow bile, and black bile — the four humours formed the foundation of Western medicine from ancient Greece to the 18th century.
